This material is intended for people without medical training who want to know more about osteochondrosis than is written in popular publications and on the websites of private clinics.Patients ask doctors of various specialties questions that characterize a complete misunderstanding of the topic of osteochondrosis.Examples of such questions are: “Why does my osteochondrosis hurt?”, “Congenital osteochondrosis was discovered, what should I do?”Perhaps the apotheosis of such illiteracy can be considered a fairly common question: “Doctor, I have the first signs of chondrosis, how scary is it?”This article is intended to structure the material about osteochondrosis, its causes, manifestations, methods of diagnosis, treatment and prevention, and answer the most frequently asked questions.Since we, without exception, are all patients with osteochondrosis, this article will be useful to everyone.
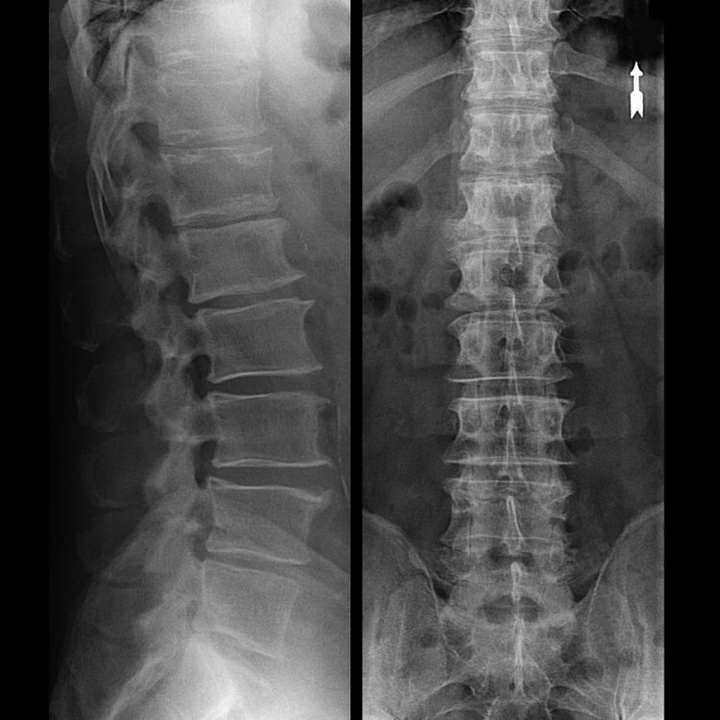
How is the intervertebral disc structured?
Each intervertebral disc consists of two different sections:
- external fibrous ring, consisting of dense fibers covering the intervertebral disc from the outside around the perimeter;
- The internal elastic component is the nucleus pulposus.
The fibers of the annulus fibrosus are very dense and elastic.Over the years, the elasticity is lost and by the age of 60 the fibrous ring becomes stiff.Between the surface of each vertebra above and below it and the intervertebral disc itself are so-called end plates, i.e. the boundary zones between the vertebra and the intervertebral disc.Through these end plates, the vertebrae grow upwards and through them the nucleus pulposus and the tissue of the intervertebral disc are diffusely nourished by the diffusion method, since the cartilage of the intervertebral disc is neither supplied with blood nor innervated.
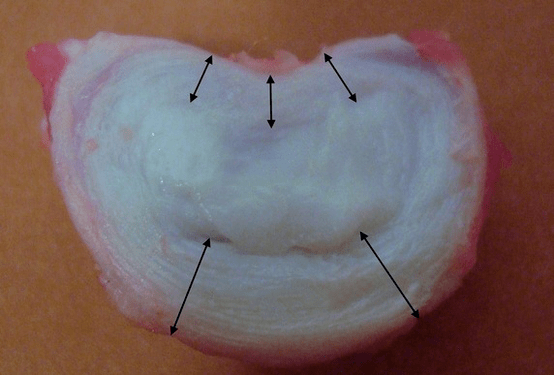
Healthy intervertebral discs in a young person are capable of high metabolic rates.If you introduce contrast into a normal disk, it will disappear from it after 20 minutes.
Studies have shown that in an adult the height of each intervertebral disc is approximately:
- 25% of the height of adjacent vertebrae in the neck region;
- 20% in the chest;
- 33% in the lumbar spine.
That is, in the lumbar region the thickness of the intervertebral discs is greatest due to the greatest load.Laboratory studies have shown that a single healthy intervertebral disc in a young person can withstand a static pressure load of up to 2.5 tons.At the age of 70, this value drops to 110 kg!That is, an “old and dried out disk” is 22 times worse at transferring the load to the sides and maintaining increased pressure in the ring.
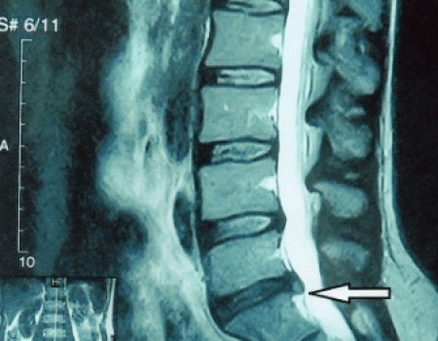
Why did this happen?Over time, the fibrous ring gradually wears away.It can no longer stretch, but only protrudes outwards, beyond the intervertebral disc, or breaks.The core stops transmitting vertical loads and converts them into radial loads.As we age, stress gradually builds up in the intervertebral discs and their structure changes.When all these processes occurring in a separate intervertebral disc are transmitted to the entire spine, a disease called osteochondrosis occurs in the clinic.Now we can start defining it.
What is Osteochondrosis?
The name of the disease is scary if it is not clear.The medical suffix “-oz” means proliferation or enlargement of a tissue: hyalinosis, fibrosis.An example would be liver cirrhosis, in which the connective tissue grows and the functional tissue, the hepatocytes, decreases in volume.There may be a buildup of pathological protein or amyloid that normally should not be present.This storage disease is then called amyloidosis.Significant enlargement of the liver can occur due to fatty degeneration, known as fatty hepatosis.
Well, it turns out that with intervertebral osteochondrosis, the cartilage tissue of the intervertebral discs increases in volume, because “chondros, χόνδρο” translated from Greek into Russian means “cartilage”?No, chondrosis, more precisely osteochondrosis, is not a storage disease.In this case, no real growth of cartilage tissue occurs;We are simply talking about a change in the configuration of the intervertebral discs under the influence of long-term physical activity and we have examined above what happens in each individual intervertebral disc.The term “osteochondrosis” was introduced into the clinical literature by A. Hilderbrandt in 1933.
Osteochondrosis refers to dystrophic-degenerative processes and is part of the normal, normal aging of the intervertebral discs.None of us are surprised that the face of a 20-year-old girl is slightly different from her face at the age of 70, but for some reason everyone believes that the spine and its intervertebral discs do not undergo the same pronounced temporary changes.Dystrophy is a nutritional disorder, and degeneration is a violation of the structure of the intervertebral discs that follows a long period of dystrophy.
Causes of osteochondrosis and its complications
The main cause of uncomplicated, physiological osteochondrosis can be seen as the way a person moves: walking upright.Of all mammals, humans are the only species on earth that walk on two legs and only move around that way.Osteochondrosis became the scourge of humanity, but we freed our hands and created civilization.Thanks to upright walking (and osteochondrosis), not only have we mastered the wheel, the alphabet and fire, but you can also sit at home in the warmth and read this article on your computer screen.
Man's closest relatives, the higher primates - chimpanzees and gorillas - sometimes stand on two legs, but this method of movement is an auxiliary method for them, and most often they still move on four legs.In order for osteochondrosis to disappear, as well as the intensive aging of the intervertebral discs, a person needs to change the way he moves and remove the constant vertical load from the spine.Dolphins, killer whales and whales do not have osteochondrosis, and dogs, cows and tigers do not have it.Your spine does not absorb long-term static and shock vertical loads because it is in a horizontal state.When humanity goes to sea and the natural means of transportation is diving, osteochondrosis is defeated.
The upright posture forced the human musculoskeletal system to evolve towards protecting the skull and brain from shock loads.But intervertebral discs – elastic cushions between the vertebrae – are not the only method of protection.A person has a springy arch of the foot, cartilage of the knee joints and physiological curvatures of the spine: two lordoses and two kyphosis.All this allows you not to “shake off” your brain even when running.
Risk factors
However, doctors are interested in the risk factors that can be modified to avoid complications of osteochondrosis, which lead to pain, discomfort, limited mobility and reduced quality of life.Let's consider these risk factors that are so often ignored by doctors, especially in private medical centers.After all, it is much more profitable to constantly treat a person than to reveal the cause of the problem, solve it and lose the patient.Here they are:
- the presence of longitudinal and transverse flat feet.Flat feet mean that the arch of the foot no longer has any spring and the shock is transmitted upwards to the spine without softening.The intervertebral discs are put under a lot of stress and collapse quickly;
- Overweight and obesity – needs no comment;
- improper lifting and carrying of heavy objects with uneven pressure on the intervertebral discs.For example, if you lift a bag of potatoes and carry it on one shoulder, the heavy load will fall on one edge of the slices and may be excessive.
- physical inactivity and a sedentary lifestyle.Above it was said that the maximum pressure on the intervertebral discs occurs when sitting, since a person never sits straight, but always bends “slightly”;
- Chronic injuries, slipping on ice, intense weight lifting, contact combat sports, heavy hats, head impacts on low ceilings, heavy clothing, carrying heavy bags in your hands.
General symptoms
The symptoms described below occur outside the localization.These are common symptoms and can occur anywhere.These include pain, movement disorders and sensory disorders.There are also vegetative-trophic disorders or specific symptoms, for example urinary tract diseases, although much rarer.Let's take a closer look at these signs.
Pain: muscle and root pain
There are two types of pain: radicular and muscular.Radicular pain is associated with compression or pressure on a protrusion or herniation of the intervertebral disc of the corresponding root at that level.Each nerve root consists of two parts: the sensory and the motor.
Depending on where exactly the hernia goes and which part of the root has been compressed, either sensory or motor disorders can occur.Sometimes both disorders occur at the same time and manifest themselves to different degrees.Pain is also a sensitivity disorder because pain is a special, specific feeling.
Radicular pain: compression radiculopathy
Radicular pain is familiar to many;it is called “neuralgia.”The swollen nerve root reacts violently to any shock and the pain is very severe, similar to an electric shock.She shoots either in the arm (from the neck) or the leg (from the lower back).Such a sharp, painful impulse is called lumbago: in the lower back it is called lumbago, in the neck it is called cervicago, a less common name.Such radicular pain requires a forced, analgesic or antalgic posture.Radicular pain occurs immediately when coughing, sneezing, crying, laughing or exerting yourself.Any shock to the swollen nerve root results in increased pain.
Muscle pain: myofascial-tonic
However, an intervertebral hernia or disc defect may not compress the nerve root, but rather injure the surrounding ligaments, fascia, and deep back muscles during movement.In this case, the pain is secondary, aching, permanent, there is stiffness in the back, and this pain is called myofascial.The source of this pain is no longer the nerve tissue, but the muscles.A muscle can only respond to any stimulus in one way: contraction.And if the stimulus lasts longer, the muscle contraction will turn into a constant spasm, which will be very painful.
A characteristic symptom of such secondary myofascial pain is increased stiffness in the neck, lower back or thoracic spine, as well as the appearance of dense, painful muscle bumps - “rolls” next to the spine, i.e. paravertebral.In such patients, back pain intensifies after several hours of “office” work with prolonged immobility, when the muscles practically cannot work and are in a spasmodic state.
Sensory disorders
When a bulge or hernia or a cramped muscle presses on the sensitive part of the nerve root, various sensory disturbances occur.They can be accompanied by pain or appear individually after the pain has already subsided.There are also completely painless forms of sensory disorders, although they are rare.
Many people are familiar with the numbness of the tips of the fingers and toes (hypesthesia or general anesthesia), reduced sensitivity of the skin in the form of long strips of the radicular type.Sometimes there is paresthesia or tingling, the feeling of “crawling goosebumps”.Sensitivity disorders most commonly occur in the feet and on the tips of the fingers and toes.Sensory disorders are quite unpleasant, but sensory disorders do not make a person disabled, but motor disorders can certainly do so.
Motor disorders in the periphery
When a motor neuron or axons that are part of the motor part of a nerve are affected, either weakness of the muscle or its complete immobility occurs.In the second case it is a complete paralysis, and in the first it is a paresis.Paresis is partial paralysis when the muscle does not work at full strength.
Most often, such diseases occur in the legs, with bulges and hernias of the lumbar spine.There are motor structures that innervate the lower leg and foot muscles.Therefore, with advanced, complicated lumbar osteochondrosis, a sprain of the foot may occur.It turns inwards, forcing the person to lift their leg up to kick with the whipping foot, this is called steppage, “cock gait”.
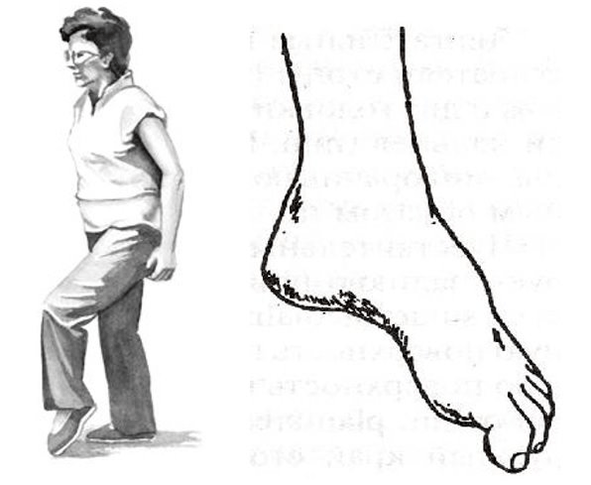
However, the whole danger of movement disorders is that they can occur in isolation and are not accompanied by pain.And if a person “doesn’t feel pain,” they may not get to the doctor on time.Therefore, it is so important for patients with progressive bulges and hernias, for example in the lumbar region, to regularly walk on their toes and heels and monitor the work of their muscles.
Local symptoms: main signs
Now let's consider specific symptoms and syndromes characteristic of cervical, thoracic and lumbar osteochondrosis.Let's go from top to bottom, from the neck region down, through the thoracic region to the lumbosacral region.
Diagnosis of osteochondrosis
In typical cases, osteochondrosis of the cervical and cervical thoracic spine occurs, as described above.Therefore, the main phase of diagnosis was and remains to identify the patient's complaints and determine the presence of accompanying muscle spasms by simply palpating the muscles along the spine.Is it possible to confirm the diagnosis of osteochondrosis by X-ray examination?
An “X-ray” of the cervical spine and even functional tests for flexion and extension do not show cartilage because its tissue allows X-rays to pass through.Nevertheless, based on the location of the vertebrae, one can draw general conclusions about the height of the intervertebral discs, the general straightening of the physiological curvature of the neck - lordosis - as well as the presence of marginal growths on the vertebrae with prolonged irritation of their surfaces by brittle and dehydrated intervertebral discs.Functional tests can confirm the diagnosis of cervical spine instability.
Since the intervertebral discs themselves are only visible using CT or MRI, magnetic resonance imaging and X-ray computed tomography are indicated to clarify the internal structure of cartilage and formations such as bulges and hernias.Thus, with the help of these methods, an accurate diagnosis is made, and the tomography result is an indication and even an actual guide for the surgical treatment of an inguinal hernia in the neurosurgical department.
Treatment of complications of osteochondrosis
We repeat once again that it is impossible to cure osteochondrosis like planned aging and dehydration of the intervertebral disc.You just can't let it complicate things:
- If symptoms of narrowing of the disc height appear, you need to move properly, not gain weight and avoid the appearance of protrusions and muscle pain.
- If you already have a lead, you need to be careful not to tear the fiber ring, i.e.
- If you have a hernia, you need to dynamically monitor it, do regular MRIs, avoid enlargement or use modern minimally invasive surgical treatment, since all conservative methods of treating exacerbation of osteochondrosis invariably leave the hernia in place and eliminate only temporary symptoms: inflammation, pain, burning and muscle spasm.
But with the slightest violation of the regime, with heavy lifting, hypothermia, injury, weight gain (in the case of the lower back), the symptoms always return.We describe how to deal with unpleasant sensations, pain and limited mobility in the back against the background of exacerbation of osteochondrosis and an existing bulge or hernia as a result of social tonic syndrome.
What to do in case of an exacerbation?
Since an acute attack of pain has occurred (for example, in the lower back), you must follow the following instructions at the premedical stage:
- completely eliminate physical activity;
- sleep on a hard mattress (orthopedic mattress or hard sofa) to avoid sagging your back;
- It is advisable to wear a semi-rigid corset to avoid sudden movements and “distortions”.
- You should place a massage pillow with plastic needle applicators on your lower back or use a Lyapko applicator.You need to keep it for 30 to 40 minutes two to three times a day.
- after that, ointments with NSAIDs, ointments with bee or snake venom can be rubbed into the lower back;
- After rubbing, on the second day, you can wrap your lower back in dry heat, for example with a belt made of dog hair.
A common mistake is not warming up on the first day.This can be a heating pad or bath procedures.At the same time, the swelling increases and with it the pain.Only when the “peak pain point” is over can you warm up.Heat then promotes the “absorption” of the swelling.This usually happens in 2-3 days.
The basis of every treatment is etiotropic therapy (elimination of the cause) and pathogenetic treatment (influence on the disease mechanisms).It is accompanied by symptomatic therapy.Vertebrogenic pain (caused by problems in the spine) looks like this:
- To reduce swelling of the muscles and spine, a salt-free diet and limiting fluid intake are indicated.You can even give a tablet of a mild potassium-sparing diuretic;
- In the acute phase of lumbar osteochondrosis, short-term treatment can be carried out with intramuscular “injections” of NSAIDs and muscle relaxants: daily.This will help relieve swelling of nervous tissue, eliminate inflammation and normalize muscle tone;
- In the subacute phase, after the maximum pain has been overcome, no more “injections” should be given and attention should be paid to strengthening agents, for example, modern drugs of group “B”.They effectively restore impaired sensitivity, reduce numbness and paresthesia.
Physiotherapeutic measures continue, the time has come for exercise therapy for osteochondrosis.Its task is to normalize blood circulation and muscle tone when swelling and inflammation have already subsided, but muscle spasm has not yet completely subsided.
Kinesiotherapy (exercise treatment) involves therapeutic exercises and swimming.Gymnastics for osteochondrosis of the cervical spine is aimed not at the intervertebral discs at all, but at the surrounding muscles.Its task is to relieve tonic spasms, improve blood circulation, and also normalize venous outflow.This leads to a reduction in muscle tone, a reduction in pain intensity and stiffness in the back.
Exercises for osteochondrosis must be performed on “warmed up muscles” after a light general warm-up.The most important therapeutic factor is movement, not the degree of muscle contraction.Therefore, to avoid relapse, the use of weights is not permitted;A gymnastics mat and a gymnastics stick are used.With their help, you can effectively restore freedom of movement.
Rubbing ointments and using the Kuznetsov applicator continues.Swimming, underwater massage, Charcot shower are shown.At the stage of subsiding exacerbation, drugs for home magnetic therapy and physiotherapy are indicated.
Usually treatment lasts no more than a week, but in some cases osteochondrosis can manifest itself with such dangerous symptoms that urgent surgery may be required.
About Shants' collar
In the early stages, in the acute stage, it is necessary to protect the neck from unnecessary movements.The Shants collar is ideal for this.Many people make two mistakes when purchasing this collar.They do not choose it according to their size, so it simply does not fulfill its function and causes discomfort.
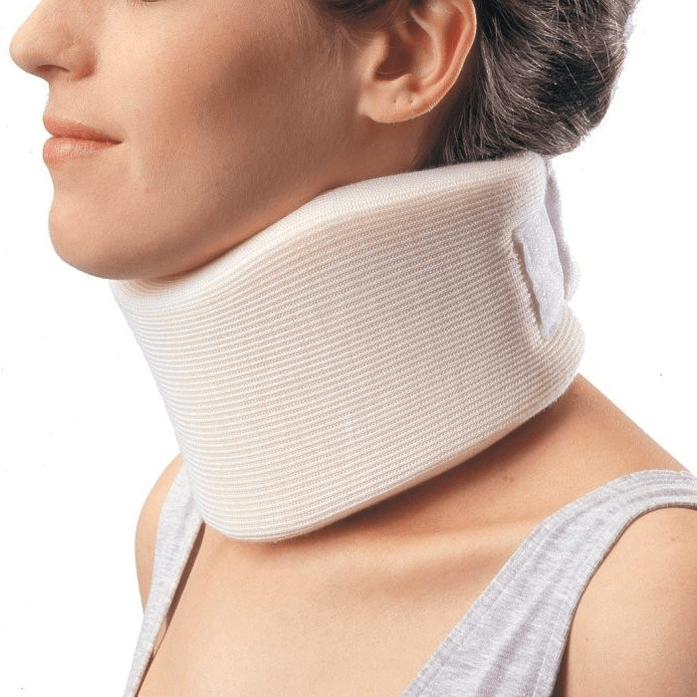
The second common mistake is wearing it for a long period of time for prophylactic purposes.This leads to weak neck muscles and only causes more problems.There are only two indications under which a collar may be worn:
- the appearance of acute pain in the neck, stiffness and pain spreading to the head;
- if you, in full health, do physical work that risks “straining” your neck and making it worse.This is, for example, repairing a car when you lie down under it, or cleaning windows when you have to reach out and assume awkward positions.
The collar should not be worn for more than 2-3 days, as prolonged wear may cause venous congestion in the neck muscles at a time when the patient needs to be activated.An analogue of the Shants collar for the lower back is a semi-rigid corset purchased in an orthopedic salon.
Surgical treatment or conservative measures?
It is advisable that every patient undergo an MRI and consult a neurosurgeon after the progression of symptoms and in the presence of complications.Modern minimally invasive operations enable the safe removal of larger hernias, without a long hospital stay, without lying down for several days and without affecting the quality of life, as they are carried out using modern video endoscopy, radio frequency, laser technology or cold plasma.They can evaporate part of the core and lower the pressure, reducing the risk of a hernia.And you can radically eliminate the defect by eliminating it completely.
There is no need to be afraid of hernia surgery;These are no longer the same as the earlier open operations of the 80s and 90s of the last century with muscle dissection, blood loss and a subsequent long recovery period.They are more like a small puncture under X-ray control and subsequent use of modern technology.
Prevention of osteochondrosis and its complications
Osteochondrosis, including complicated ones, the symptoms and treatment of which we discussed above, is for the most part not a disease, but simply a manifestation of inevitable aging and premature “shrinkage” of intervertebral discs.Osteochondrosis needs little to never bother us:
- Avoid hypothermia, especially in fall and spring, and fall in winter.
- Do not lift weights and only carry loads in your backpack with your back straight.
- drink more clean water;
- Don't get fat, your weight should correspond to your height;
- Treat flat feet, if present;
- Do physical exercises regularly;
- performing exercises that relieve strain on the back (swimming);
- give up bad habits;
- Alternation between psychological stress and physical activity.After every hour and a half of mental work, it is recommended to change the type of activity to physical work;
- You can regularly take at least one x-ray of the lumbar spine in two projections or an MRI to determine whether the hernia, if any, is progressing;
By following these simple recommendations, you can keep your back healthy and mobile throughout your life.
























